Let's Talk Pulse Oximetry
We have all seen them - either the sticker or clip on your finger attached to the vitals machine. The elusive pulse oximeter. There are also small portable ones that are the size of a snack-sized snickers bar.
What does a pulse oximeter do for asthma?
A pulse oximeter measures 2 different things: heart rate and oxygen saturation in the blood.1 The heart rate part is pretty straight forward. It picks up on the lub-dub of your heart and, in turn, shows the number on the screen.2
The oxygen saturation reading indicates the percentage of hemoglobin molecules in arterial blood that are saturated with oxygen. It works by shining a light through your finger and the sensors detect how much oxygen is in your blood based on the way the light passes through your finger. Since the oximeter detects the saturation peripherally on a finger, toe, or earlobe, the result is recorded as the peripheral oxygen saturation, known as the SpO2.2
Nowadays pulse oximeters are readily available to purchase both online and in most pharmacies to purchase over the counter. Back when I started my career in respiratory therapy many years ago I had to show my license in order to be able to purchase one without a prescription. That's not the case anymore.
Pulse oximeter limitations
There are limitations to pulse oximeters, one of the biggest ones being that not all pulse oximeters are created equal. Oximeters that are less expensive than the hospital-grade ones often do not have the accuracy that those in in the hospital or that your respiratory therapist (such as myself) has in their pockets.3,4
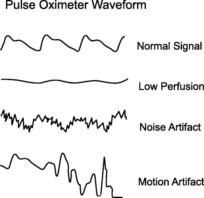
There are also many things that can affect the reading and give a false one, such as nail polish, poor circulation to the extremities, movement (or shakiness), and cold hand, which are all things to take into consideration when getting a reading. Also, if your pulse oximeter has a display that shows a waveform, you want to see that the waveform is uniform with the hills and valleys equal as it goes across the screen while giving a reading.4
Here is a really good graphic that shows a good pulse oximeter reading vs an inaccurate one:
Understanding pulse oximeters for asthma
Oxygen saturation is not a good indication of how bad your asthma flare-up is. Asthmatics are notoriously good oxygen compensators and can have near-normal or completely normal oxygen stats during the midst of a severe asthma attack. Asthma is a disease of the airways, not the little air sacs (alveoli) where the gas exchange itself takes place. So even if your airways are very constricted and tight, often enough oxygen is able to pass through to your blood and therefore show a normal or near-normal oxygen saturation that does not require oxygen therapy.5
Now if you have been working really hard to breathe for a time (which can be days if you're in the middle of a bad flare-up) your body will eventually tire out as you won't be able to compensate anymore and your oxygen levels will start to rapidly drop.5,6
If your oxygen levels are in the normal range (textbook normal range for oxygen saturations is 92% to 100%) it definitely does not mean you aren't suffering nor having a potentially severe asthma attack. It just means that you are still able to oxygenate your body. When an asthmatic’s oxygen levels start to trend downward is when immediate medical attention is required (if you aren't already at the hospital or doctors office) as it can be a sign of impending respiratory failure.6,7
Be aware of your symptoms
I want to really stress that symptoms trump numbers. I'll say it again: SYMPTOMS TRUMP NUMBERS. If you are having difficulty breathing, consider that before the number you see on a screen. I teach new respiratory therapists, nurses, and interns that you always treat the patient and not the numbers you see.
While pulse oximeters are great and can be a handy little tool for asthma monitoring, knowing exactly what they do and their limitations can be helpful.

Join the conversation